Hi everyone 👋,
Happy Monday!
Unlike last week this is a jam-packed week for research! The newsletter is a little bit longer than normal as a result. The Long Covid paper I highlighted this week is the most comprehensive Long Covid paper I have read.
For those who are interested, here is my thread on Metformin.
📰 Media
Add This to the List of Long COVID Symptoms: Stigma
From WebMD:
Most people with long COVID find they’re facing stigma due to their condition, according to a new report from researchers in the United Kingdom. In short: Relatives and friends may not believe they’re truly sick.
“After years of working on HIV-related stigma, I was shocked to see how many people were turning a blind eye to and dismissing the difficulties experienced by people with long COVID,”
Azola calls the medical community a major problem when it comes to dealing with long COVID.
Long COVID researchers in CT to get part of $10 million in federal funding
From CTPublic:
The federal government recently allocated $10 million for long COVID research, and some of that money is arriving in Connecticut, including at Yale and UConn.
My take: I only included this to help remind us all that the federal spending for Long Covid is happening, albeit at a slower pace than expected.
Long Covid can be debilitating, even for healthy kids
From the CNN:
“Looking at our first 60 patients that came to our clinic, we found that about 13% of our patients had these functional neurologic deficits.”
Murrow and Edwards remind parents that the best way to protect kids from long Covid is to keep them from catching the virus in the first place
🔍 Research
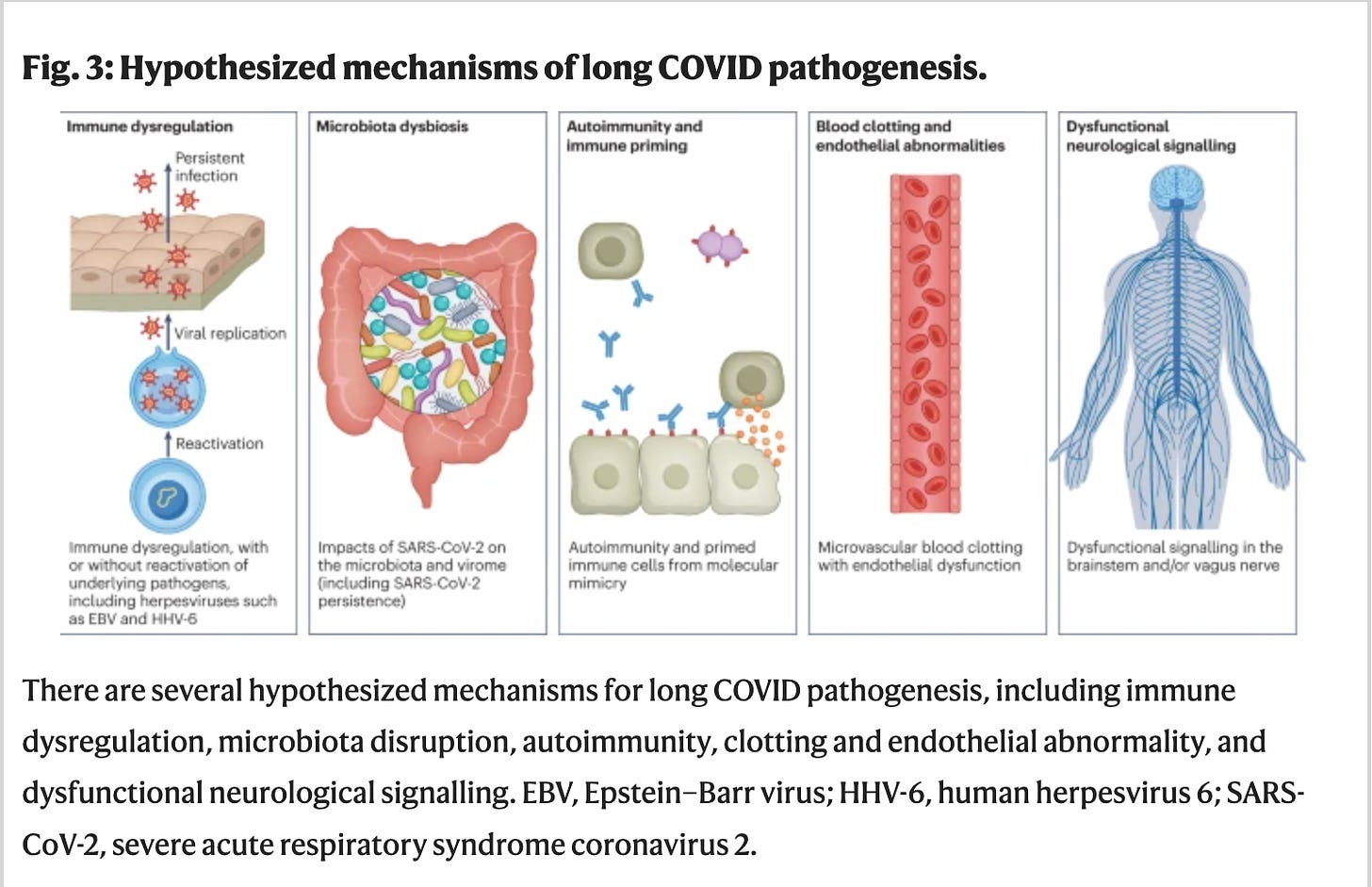
Long COVID: major findings, mechanisms and recommendations
🚨This is a must read!!!
From Nature:
Some of the findings include:
Studies looking at immune dysregulation in individuals with long COVID who had mild acute COVID-19 have found T cell alterations, including exhausted T cells, reduced CD4+ and CD8+ effector memory cell numbers
Multiple studies have found elevated levels of autoantibodies in long COVID
Reactivated viruses, including EBV and HHV-6, have been found in patients with long COVID
Several studies have shown low or no SARS-CoV-2 antibody production and other insufficient immune responses in the acute stage of COVID-19
indicated a significantly increased risk of a variety of cardiovascular diseases, including heart failure, dysrhythmias and stroke
In a meta-analysis, fatigue was found in 32% and cognitive impairment was found in 22% of patients with COVID-19 at 12 weeks after infection
Many researchers have commented on the similarity between ME/CFS and long COVID; around half of individuals with long COVID are estimated to meet the criteria for ME/CFS
Long COVID gastrointestinal symptoms include nausea, abdominal pain, loss of appetite, heartburn and constipation. The gut microbiota composition is significantly altered in patients with COVID-19, and gut microbiota dysbiosis is also a key component of ME/CFS
The impact of vaccination on long COVID symptoms in people who had already developed long COVID differs among patients, with 16.7% of patients experiencing a relief of symptoms, 21.4% experiencing a worsening of symptoms and the remainder experiencing unchanged symptoms
My Take: This is the most comprehensive review to-date of Long Covid. It is lengthy but most definitely worth a read. Hopefully this spurs a lot of research.
Converging Evidence of Similar Symptomatology of ME/CFS and PASC Indicating Multisystemic Dyshomeostasis
From MDPI:
The current hypothesis is unique in proposing that, unlike disorders that typically return the equilibrium to a previously established or fixed set point or range, ME/CFS and PASC involve a changed set point in which the organism is pushed towards a pathophysiological state in which the disequilibrium is unable to reset.
The pattern of symptoms for ME/CFS and PASC is highly similar. Using a psychometrically reliable and validated measure, the correlation in mean symptom scores across 62 symptoms is 0.902.
Circulating anti-nuclear autoantibodies in COVID-19 survivors predict long COVID symptoms
From ERS:
While most of the healthy controls did not have IgG autoantibodies, approximately one-third of the convalescent COVID-19 group had at least one autoreactive IgG.
Positive correlations were found between various ANAs/ENAs and inflammatory mediators: CRP, ICAM-1, VCAM-1, IL-8 and TNF-α
Second, high titres of circulating ANAs/ENAs were maintained up to 6 months post-recovery, but were significantly attenuated by 12 months, although several pathogenic ANAs/ENAs are still detectable in up to 30% of COVID survivors at 12 months.
My Take: This opens up some questions. Why do some people develop autoantibodies while others do not? Why they disappear for some people but not for others?
Chronic Fatigue, Depression and Anxiety Symptoms in Long COVID Are Strongly Predicted by Neuroimmune and Neuro-Oxidative Pathways Which Are Caused by the Inflammation during Acute Infection
Definition: NLRP3 is an intracellular sensor that detects a broad range of microbial motifs, endogenous danger signals and environmental irritants, resulting in the formation and activation of the NLRP3 inflammasome. NLRP3 inflammasome leads to caspase 1-dependent release of the pro-inflammatory cytokines IL-1β and IL-18 (source)
From MDPI:
High peak BT(body temperature) and lowered SpO2 during the acute phase of COVID-19 are associated with the development of the physio-affective phenome of long COVID disease, and these effects are partially explained by increased NT through activation of the NLRP3 inflammasome, a mild inflammatory response, increased chlorinative stress, and lowered total Ca levels.
The results confirm that … symptoms, … share common immune–inflammatory pathways, as reviewed in the introduction
IL-1β is necessary to start and maintain the immune–inflammatory reactions in the central nervous system (CNS) and may impact the integrity of the blood–brain barrier (BBB), leading to leakage of peripheral immune cells into the CNS Moreover, IL1β mediates microglia and astrocyte activation, resulting in infiltration of T cells into the CNS, thus augmenting the pro-inflammatory state by producing IL-6 and TNF-α along with neurotoxic metabolites, enhancing excitotoxicity and neuronal damage
My Take: This was my first time hearing of NLRP3. I’d be interested to see long-term studies into this and microglia with Long Covid.
The Effect of COVID-19 on Long-Term Cardiac Function in Patients With Chronic Heart Failure
Definition: Left ventricular ejection fraction - measures your heart’s ability to pump oxygen-rich blood out to your body. In a healthy heart, the fraction is a higher number.(source)
From Kardiologiia:
This study showed that COVID-19 in the long term can influence the course of Chronic Heart Failure; in this process, HF patients with Left ventricular ejection fraction <50% have progression of systolic dysfunction and PASP, whereas patients with Left ventricular ejection fraction>50% have an isolated increase in PASP(pulmonary artery systolic pressure).
🩺 Hope & Potential Treatments
Nebivolol: an effective option against long-lasting dyspnoea following COVID-19 pneumonia - a pivotal double-blind, cross-over controlled study
From MRM:
effective in increasing pulmonary capillary blood volume and the corresponding dyspnoea substantially, both persisting for several weeks after hospital discharge
Stellate Ganglion Block for Long COVID Symptom Management: A Case Report
From Cureus:
This case report showcases the potential effectiveness in the treatment of other prominent long COVID symptoms including fatigue, PEM, SOB, and GI disturbances.
SGB may treat dysautonomia by increasing both cerebral and regional blood flow, in turn, resetting the autonomic nervous system function
My Take: Would definitely be interested to see a clinical trial into SGB.



As usual, a truly excellent review of the research. Thank you so much for the service you're providing
Good afternoon,
Just discovered the newsletter today via Reddit. Haven't had a chance to review the past weeklies, but it appears to be very informative, and I'd like to thank you for all the effort.
I was particularly interested in the note about Nebivolol. Primarily because I've been on it(5mg) for about six months; prescribed by my cardiologist as part of my heart meds program. I'm afraid I can't report anything positive on reducing my shortness of breath since I began taking it. Just an FYI.