Hi everyone,
Happy Monday!
I experimented with some longer summaries this week, if this is not what people want I can change it!
Possibly looking for someone who wants to collaborate on this newsletter and maybe some other research stuff for another Twitter account I am thinking about making. Email me or DM me on Twitter if interested!
Let’s get into things!
📰 Media
NIH RECOVER research identifies potential long COVID disparities
From NIH:
Black and Hispanic Americans appear to experience more symptoms and health problems related to long COVID(link is external), a lay term that captures an array of symptoms and health problems, than white people, but are not as likely to be diagnosed with the condition, according to new research funded by the National Institutes of Health.
In the months following infection, Black adults with severe disease were more likely than white adults to be diagnosed with diabetes and experience headaches, chest pain and joint pain, but less likely to have sleep disorders, cognitive problems, or fatigue. Similarly, Hispanic adults who required hospital care were more likely than white adults to have headaches, shortness of breath, joint paint, and chest pain, but less likely to have sleep disorders, cognitive problems, or fatigue.
Children and teens were more likely to experience gastrointestinal and upper respiratory problems, including stomach aches and coughing. Adults ages 21-45 commonly experienced neurological problems, such as brain fog and fatigue. Adults ages 66 and older were more likely to have coexisting conditions, such as heart problems and diabetes, which the authors suspect is more likely present because of age than long COVID.
The haunting brain science of long Covid
From Statnews:
Matt Fitzgerald used to bike up and down 3,500 feet through the Santa Ana Mountains on three-hour rides just for fun. Now, nine months after being infected with SARS-CoV-2, the virus that causes Covid-19, he can’t muster walking on flat surfaces for 20 minutes without days of exhaustion.
It is now clear from U.S. and U.K. investigations of approximately 2,000 previously hospitalized Covid patients that six months later more than half have problems managing finances and paying bills as well as completing everyday activities like preparing meals, bathing, getting dressed, or walking across a room.
Autopsy studies show that the virus can persist in some people for many months even though they have no symptoms and test negative for the virus.
A study from the National Institutes of Health of 44 complete autopsies mapped and quantified the distribution of SARS-CoV-2 and showed it was widely distributed throughout the body, including in the hypothalamus and cerebellum in the brain and neurons in the spinal cord.
People living with long COVID explain how the disease changed their lives
From PBS:
Last fall, President Biden said the pandemic was over. '
And judging by how most Americans are living their lives, they agree. That's even though this virus is still killing about 2,000 Americans every single week.
Physically, long COVID has absolutely just ruined my life. I mean, it really has. There's no other way to say that.
Now I have these debilitating symptoms. And there's no treatment and no cure for it. And doctors don't know what to do with you.
🔍 Research
Deep dive: microclots in long COVID
From the LCbreakdown:
A group of researchers have found miniature blood clots in acute COVID-19 patients, as well as patients with long COVID. The clots are made up of a protein called fibrin that has taken on an anomalous, or amyloid, structure.
Researchers found that the S1 portion of the spike protein is sufficient to induce microclot formation in samples from healthy patients.
While both acute and long COVID patients have microclots, the clots in long COVID patients contained more inflammatory markers that can also contribute to altered coagulation processes.
Preliminary reports indicate 100% of long COVID patients have detectable microclots.
Microclots could serve as a type of “underlying mechanism” in long COVID, as it intersects with several other lines of research including:
Metabolic dysfunction
Immune dysregulation
Endothelial disruption
Viral persistence
Vaccine injury
My Take: Definitely recommend everyone read this one! Extremely in-depth and thorough review!Why we need a deeper understanding of the pathophysiology of long COVID
From the Lancet:
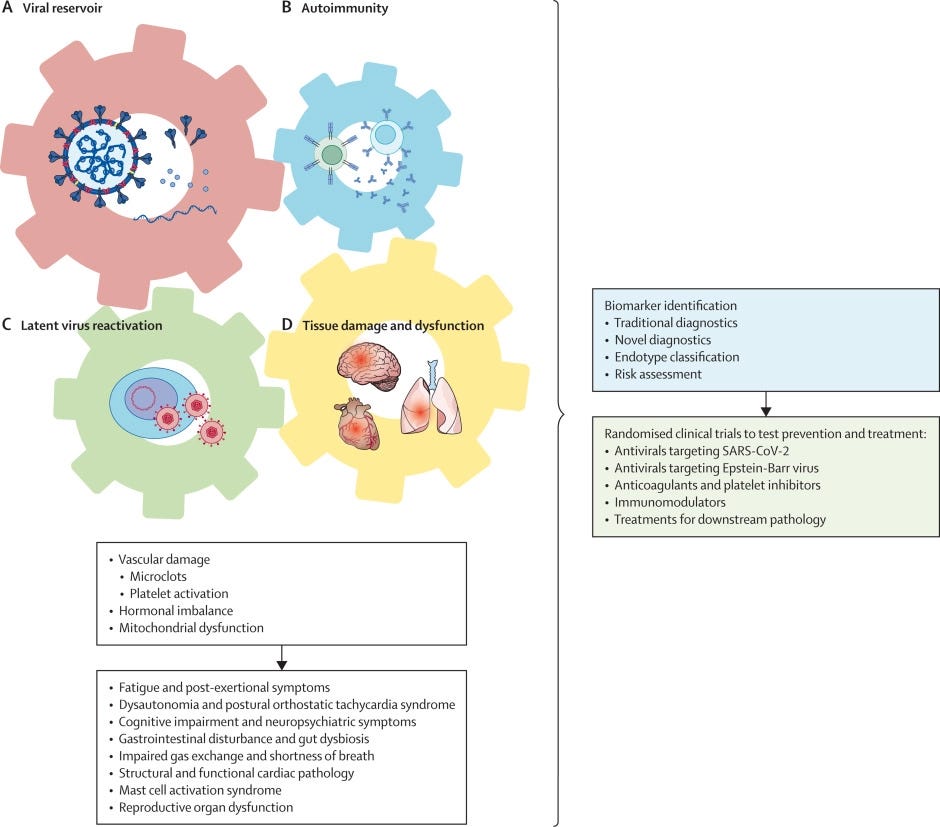
Long COVID is a condition that affects a significant number of individuals globally, with more than 65 million people estimated to be living with it. The condition is a blanket diagnosis that represents a heterogeneous set of pathophysiological processes…
Despite the multifactorial pathogenesis, available data show that long COVID is an organic post-acute infection syndrome with clear physiological dysfunction that is often not consistently apparent using standard medical diagnostic tests. The discrepancy highlights the need for a new generation of more sensitive testing procedures for people with PAIS. The identification of biomarkers for long COVID and distinct endotypes driven by different root causes will be crucial for identifying predisposing factors and implementing evidence-based policies.
Ideally, potential therapies should be assessed in double-blinded, placebo-controlled, randomized clinical trials. However, such studies are quite costly, labor-intensive, and require substantial government, regulatory, and industry support.
My Take: A thought provoking piece! Akiko Iwasaki & David Putrino are at the forefront of Long Covid research.Sex-related patient-reported brain fog symptoms in non-hospitalised COVID-19 patients
From the Polish Journal of Neurology and Neurosurgery:
Neurological manifestations have been observed not only throughout the acute phase of illness [5–9] but also during the post-infection period [10, 11]."Among these persistent symptoms, cognitive, memory and concentration disturbances have been reported by approximately one in four patients with a previous SARS-CoV-2 infection [12], and their presence interfered with daily activities and delayed the chance of complete recovery [13, 14].
Women more often reported problems with writing, reading, counting and communication of thoughts.They also more often declared difficulties with answering questions in an understandable/unambiguous manner between four and 12 weeks after the onset of COVID-19, and in recalling new information up to 12 weeks after infection. A large meta-analysis of 20 studies on more than 13,000 hospitalised patients showed that female sex increased the risk of any new or persistent mental health symptom 1.67-fold after COVID-19 [23].
Transcriptionally active nasopharyngeal commensals and opportunistic microbial dynamics define mild symptoms in the COVID 19 vaccination breakthroughs
From PLOS Pathogens:
Multiple vaccines have been developed to effectively control the ongoing pandemic. According to Amanatidou et al., breakthrough infections are caused by four major factors: vaccination parameters, viral traits, immune characteristics and host determinants. Whether the human resident nasopharyngeal microbes, especially transcriptionally active microbes (TAMs), play a role in vaccination breakthrough needs to be deciphered
Although limited, it has been highlighted that vaccine-induced immune responses can be modulated by alterations in microbial composition.
These findings emphasize the necessity of identifying the factors, such as the use of antibiotics and probiotics, before or during vaccination, which may either modulate the host microbiota to boost vaccine efficacy or cause reinfections.
Thus, through the present cross-sectional study, we have explored and elucidated the functional role of transcriptionally active microbes (TAMs) using dual RNA-Sequencing (RNA-Seq) and metagenomic analysis of the nasopharyngeal microbiome in the SARS-CoV-2 infected individuals, between cohort of vaccination breakthrough and non-vaccinated infections.
Growing evidence suggests that microbes and their molecules influence the immune response to vaccination against viruses such as influenza and SARS...
My Take: This is not necessarily long covid related but thought it was super interesting. It seems like the microbiome has a hand in everything...A case of post-COVID-19 myalgic encephalomyelitis/chronic fatigue syndrome characterized by post-exertional malaise and low serum acylcarnitine level
From the Wiley Online Library:
Currently, no blood tests or imaging studies provide a definitive diagnosis of ME/CFS, although such procedures may serve to rule out alternative competing diagnoses. Given the difficulty in diagnosing ME/CFS, patients who have recovered from the acute phase of COVID-19 but who still present with symptoms often wait several years before receiving appropriate care for ME/CFS; this prolonged period without an effective diagnosis may contribute to the 30% of patients who
Of the proposed criteria (Table 3), two factors were especially salient for our patient and, therefore, were pivotal in directing our attention to the possibility of ME/CFS in the context of post-COVID recovery.. Viral infections are known to disrupt the mitochondrial fatty acid oxidation cascade, thus potentially contributing to a decrease in serum acylcarnitine. Consistent with this, research indicates that the rates of ME/CFS increase in conjunction with viral infections, including SARS-CoV-2 infection.
🩺 Hope & Potential Treatments
Human Umbilical Cord Blood (RegeneCyte) Infusion in Patients With Post-COVID Syndrome
From Clinicialtrials.gov
New clinical trial in the works


Hi, I'm wondering if you have had a look at my posts related to Long COVID. They are based on my personal experience with Long COVID and an hypothesis of mitochondrial dysfunction exacerbated by chronic inflammation. I'm wondering if you would be interested in any form of cross posting?
Kind regards, Mardi Crane-Godreau, PhD
Can you share your email? I’d love to contact you about helping.