Long Covid Weekly #44: MillionsMissing, Previous (non covid-19)Coronavirus infections causing issues & more
Hi everyone
Welcome to the latest edition of our Long Covid newsletter. In this issue, we delve into some of the latest research on the topic, including studies on the potential causes of lasting pain and the association between SARS-CoV-2 infection and persistence with Long Covid. We also investigate the challenges facing Long Covid patients as they struggle to find solutions and demand answers from their medical providers. Plus, we explore the immunologic imprinting of previous Coronaviruses and its effects on neurologic sequelae.
Media
Article: Why aren’t there better treatments for long COVID?
SUMMARY:
The clues they have suggest that patients would likely benefit from pharmaceutical therapies, but without a known mechanism or definitive diagnostics, government agencies and pharmaceutical companies seem reluctant to develop and test treatments.
That leaves patients in a terrible lurch.
Scientists don’t know why some patients with COVID fail to get better, though a number of avenues are being explored.
With the government effort lagging, citizen-scientists, academic researchers, small companies, nonprofits such as PolyBio, and patients themselves have stepped into the breach.
Article: New study suggests that SARS-CoV-2 might induce lasting pain in unique way
DEFINITIONS:
Sensory-related symptoms: issues related to touch, pressure, temperature, pain, or tingling throughout the body.
SUMMARY:
Researchers have found that SARS-CoV-2-mediated disease may cause lasting pain by affecting genes associated with neurodegeneration and pain-related pathways.
They suggest that molecular pathways specific to the virus should be targeted to manage these symptoms.
The researchers studied the effects of infection on sensitivity to touch in an experimental model infected with SARS-CoV-2.
New genes and pathways affected by the virus have been identified weeks after infection. This is expected to provide a better understanding of the gene expression changes in sensory ganglia.
SUMMARY:
For long COVID patients, the pandemic is far from over.
The U.S. public health emergency expires today, and many fear that their struggle – to be recognized and treated within the nation’s fragmented health care system – is only beginning.
When it comes to finding expert guidance and treatment for the complex tangle of disorders and illnesses, “COVID is a full-time job,” said long COVID patient Liza Fisher.
Fisher was among the first patients to be seen at a post-COVID care center in San Antonio, Texas, that opened in summer 2020.
Similar clinics have popped up around the nation that offer a hub of care where pulmonologists, cardiologists, neurologists and more specialists examine the complex nature of long COVID.
Article: House Democrat demands answers on long Covid research - STAT
DEFINITIONS:
National Institutes of Health (NIH): is the primary health agency of the US Government responsible for carrying out and funding medical research.
SUMMARY:
Rep. Anna Eshoo, the House Energy and Commerce health subcommittee’s top Democrat, is demanding answers from the National Institutes of Health (NIH) about its slow progress on long COVID research.
Eshoo has highlighted the agency's delays in enrolling clinical trials, the lack of relief for patients, the exclusion of long Covid from the White House’s Next Gen program, and the NIH’s nearly exhausted budget for studying long Covid.
The investigation found the NIH’s $1.2 billion effort to study long Covid has yielded little useful information for patients, despite facing delays in starting clinical trials for treatment.
Eshoo is requesting information about NIH’s remaining budget on long Covid, plans for future spending, and specific dates of clinical trial enrollment.
My Take: .
The NIH’s lack of progress is concerning, and patients deserve more information, better treatments, and better support from the agency.
Overall, this article shows the critical need for transparency and more funding to combat long Covid, given its massive/significant implications on the health sector.
DEFINITIONS:
Obstructive sleep apnea: occurs when the upper airway becomes blocked during sleep, which interrupts breathing.
The condition affects about 1 in 8 adults but is often underdiagnosed.
SUMMARY:
Among people who have had COVID-19, adults with obstructive sleep apnea were more likely to experience long-term symptoms suggestive of long COVID than those without the sleep disorder.
Multiple analyses of electronic health records (EHR) uncovered adults with sleep apnea may have up to a 75% higher risk of developing long COVID.
The findings may also strengthen understanding of why some people are more likely to develop the post-viral syndrome after acute infection.
The research, which came from EHR data of more than 2.2 million Americans with COVID-19, suggests close monitoring after a COVID-19 infection may help adults with sleep apnea.
Research
DEFINITIONS:
Dysbiosis: a microbial imbalance or maladaptation on or inside the body, such as an impaired microbiota.
Fecal Microbiota Transplantation (FMT): a procedure that involves the transplantation of fecal matter from a healthy donor into the digestive tract of a patient.
PICRUSt2: a tool used for predictive functional profiling of microbial communities.
SUMMARY:
The study aimed to analyze the gut microbiota diversity in Indian COVID-19 patients and identify the key signatures in the gut microbial ecology in patients with severe COVID-19 disease as well as in response to different therapies.
The relative abundance of Firmicutes was the highest in severe COVID-19 patients, followed by Actinobacteria, Proteobacteria, Bacteroides, Cyanobacteria, and Desulfobacterota.
The Lachnospiraceae family was found to be the most differentially relatively abundant taxa between patients with mild and severe COVID-19.
The metabolic capacity of the microbiome was inferred using microbial diversity obtained from the 16S rRNA gene amplicon data by PICRUSt2 software.
My Take:
The findings emphasize that the gut microbiota might play a crucial role in COVID-19 pathogenesis, and modulation of the gut microbiota might be an innovative therapeutic approach for COVID-19 patients.
DEFINITIONS:
Systems serology approach: It is an in-depth analysis of the antibody and the B-cell responses, to identify the specific mechanisms of protection that elicit vaccination or natural infection.
humoral immunity: It is a type of immunity that is mediated by macromolecules found in the extracellular fluids such as secreted antibodies, complement proteins, and certain antimicrobial peptides.
SUMMARY:
Emerging data suggest that compromised peripheral SARS-CoV-2 immunity may lead to development of neuroPASC due to partial or delayed viral clearance and persistent neuroinflammation.
Using a high throughput systems serology approach, distinctive humoral signatures were identified across individuals with and without neuroPASC.
Individuals with neuroPASC were characterized by a diminished systemic response to SARS-CoV-2, in contrast with an expanded systemic response to common Coronaviruses.
stronger serum SARS-CoV-2 responses are clearly linked to better outcomes in neuroPASC individuals, likely through improved clearance or control of the infection.
These data point to a clear selective transfer of antibodies to specific pathogens to the brain likely related to the … recently generated, potentially more inflammatory antibodies, to fight infection in the brain.
My Take:
Understanding the molecular mechanisms underlying post-acute neurological complications can revolutionize patient care and the development of disease-modifying therapies.
I found this one super interesting, basically strong reactions to prior coronaviruses led to worse downstream outcomes?
DEFINITIONS:
Immunosuppressive type 1 regulatory T-cells (TR1): adaptive bystander cells that can reestablish tolerance in immune-mediated diseases.
SUMMARY:
T-cell dysfunction, cytokine imbalance, and impaired autoimmunity have been reported in PCS.
A prospective, controlled study found that unvaccinated COVID-19 convalescents with PCS have a distribution of T-cell subpopulations, cytokine levels, and p DC activation that suggests immunological alterations of both immune activation and immunosuppression.
Our analysis revealed that neither levels of SARS-CoV-2 IgG or cytokines nor quantitative and qualitative features of CD4+ T-cells alone allowed an identification of PCS+.
However, distinct patterns of altered immune responses were most apparent in PCS+ as early as 6 weeks after symptom onset, which persisted until the seventh month.
In response to the increased inflammation observed in PCS, the immune system appears to initiate immunosuppressive countermeasures.
The study did not find specific diagnostic biomarkers for PCS but suggests that IL-4 and TR1 may provide potential directions for future epidemiological investigations and targeted treatments.
Article: The plasma metabolome of long COVID-19 patients two years after infection | medRxiv
SUMMARY:
In the present work, our aim was to evaluate the persistence of long-term metabolic alterations in post-COVID-19 patients, as well as to measure immune markers that, when chronically produced, can trigger autoimmune diseases.
Our results revealed that 50% of analyzed plasma metabolites showed statistical differences between COVID-19 and post-COVID-19 phases. One of the most dysregulated metabolites was glucose.
This indicates that, although lower in magnitude, the inflammatory conditions attributable to the hyperactivation of this metabolic pathway are still present and may account for some persistent physiological symptoms in these patients.
Alterations in lipid metabolism are evident in most post-COVID-19 patients.
Mitochondrial dysfunction, redox state imbalance, impaired energy metabolism, and chronic immune dysregulation are considered to be the main hallmarks of long COVID, even two years after acute COVID-19 infection.
My Take:
Super interesting read…
SUMMARY:
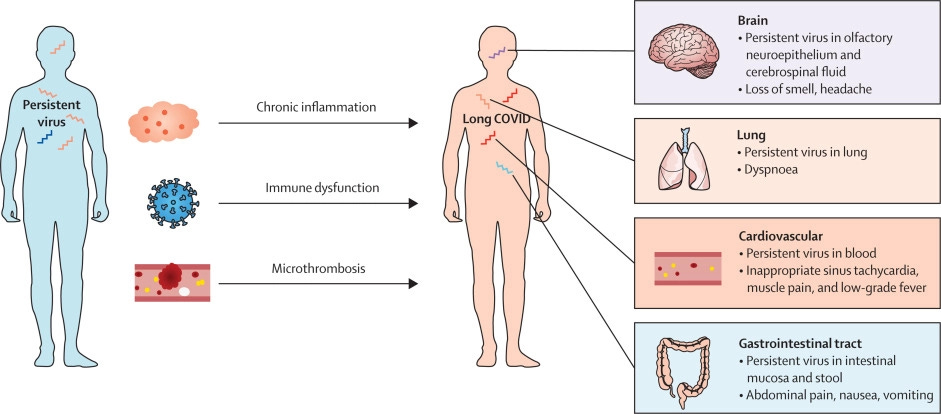
The article discusses the persistence of SARS-CoV-2 virus and its correlation with long COVID, which can affect anyone exposed to the virus.
The duration of SARS-CoV-2 virus in patients can persist considerably longer than suggested by PCR-negative tests on nasopharyngeal swabs or bronchoalveolar lavage fluids.
In another study, the circulating SARS-CoV-2 components, spike protein, and viral RNA fragments persisted for up to 1 year or longer after SARS-CoV-2 acute infection in patients with long COVID, whereas these viral components decreased or were totally absent in convalescent patients with COVID-19, as shown by ddPCR and spike protein ELISA techniques.
Rapid viral elimination in patients with persistent SARS-CoV-2 virus might be crucial as reinfection further increases risks of death, hospitalization, and sequelae in multiple organ systems in the acute and post-acute phases.
My Take:
The article highlights the need to comprehensively understand the pathogenesis of long COVID related to the persistence of SARS-CoV-2 virus to help develop and implement future strategies for prevention, treatment, and health-resource planning.
Hope
A protest on Friday in Washington D.C. by MEAction and Body Politic, drew attention to the #MillionsMissing from life due to ME/CFS caused by post-viral illnesses, including Long Covid.
Rows and rows of cots lined up at the Washington Monument represented beds, as a symbolic protest that, although the emergency response has ended, the pandemic is not over for millions of Americans who have ME and Long Covid
The ME/CFS community has partnered closely with the Long Covid community since Long Covid began.
Now, up to 1/2 of patients with Long Covid meet the diagnostic criteria for ME/CFS.
The press conference included amazing patient advocates, journalists, experts and activists, who demanded bold, urgent governmental action, including much more federal research dollars, awareness campaigns, and structural support systems for people with ME/CFS, Long Covid, and associated illnesses.
Some great photos here:
Source: https://twitter.com/exceedhergrasp1/status/1657077148539052051
Clinical Trials: Top Priority for Long COVID
SUMMARY:
Drugs Proposed by Experts in Postviral Fields Should Be Prioritized
Drugs Targeting a Wide Range of Mechanisms Should Be Trialed
Behavioral Treatments, Especially Those That Have Harmed Similar Populations, Should Not Be Trialed
Endpoints should be high-impact and aim for large improvements that have clinical significance over small improvements that do not have clinical significance.
Trial Participants Should Reflect the Diversity of the Long COVID Population
Certain demographics are more likely to be affected by acute and long COVID and need to be appropriately recruited and reflected in research, including in patient engagement.





This is a vital resource for 'us' who are afflicted with a version of LC. Almost a year in for me and symptoms getting worse in certain areas. Your work gives an element of things happening. The forgotten millions of ME/CFS sufferers for many decades demonstrate sadly, what happens when another funding priority emerges, or simply, governments turn off research funding. Again, thank you for your commitment to 'us'. I am very grateful. Paul, Sydney Australia
Thanks for your newsletters.
It’s great to be able to just read the summary of the main points - rather than spend all that energy reading through and processing the article in its entirety.
At least there is research happening but it’s such a worry there isn’t enough funding being invested.
Without suitable treatments, people are at risk of trialling dangerous treatments/drugs themselves, wasting money and energy on alternate treatments which may not help and peoples mental health declining.
I desperately hope there will be some answers on day.
I’m also from Australia 🇦🇺