Hi Everyone!
In this issue, we delve into a number of new studies and articles that shed light on the long-term effects of Covid-19, including dyspnea, pain, and reduced mobility reported a year after hospitalization, the risk of post-acute sequelae associated with pre-existing conditions such as obstructive sleep apnea, and the immune mechanisms underlying Covid-19 pathology and post-acute sequelae. We also explore the impact of Covid-19 on pregnant women and fetal survivors and the potential benefits of oxygen therapy in improving heart function in Long Covid patients. Read on for these and other compelling stories.
Shoutout to Amy E. for finding up this awesome resource full of Long Covid research, in the comments of last week’s post. Definitely give it a look & let me know what you think.
I will likely be taking a break from the newsletter next week. As always, I will be posting interesting articles on my Twitter.
Media
SUMMARY:
Initial findings from a study of nearly 10,000 Americans, many of whom had COVID-19, have uncovered new details about long COVID, the post-infection set of conditions that can affect nearly every tissue and organ in the body.
The research team, funded by the National Institutes of Health, also found that long COVID was more common and severe in study participants infected before the 2021 Omicron variant.
Research continues to serve as the foundation for planned clinical trials, whose interventions are rooted in many of the symptoms outlined in this study.
They assessed more than 30 symptoms across multiple body areas and organs and applied statistical analyses that identified 12 symptoms that most set apart those with and without long COVID: post-exertional malaise, fatigue, brain fog, dizziness, gastrointestinal symptoms, heart palpitations, issues with sexual desire or capacity, loss of smell or taste, thirst, chronic cough, chest pain, and abnormal movements.
My Take:
This is a pretty monumental research drop, the media frenzy after this was unlike anything I have seen for Long Covid Research
By identifying the most common symptoms and potential subgroups and developing a symptom-based scoring system, the researchers aspire to improve future diagnoses and treatments.
Article: Dyspnea, pain, reduced mobility reported 1 year after COVID-19 hospitalization
DEFINITIONS:
Dyspnea is the experience of shortness of breath or difficulty breathing.
SUMMARY:
Dyspnea, pain and reduced mobility were commonly reported by survivors of COVID-19 1 year after their hospitalization, according to researchers.
Comorbidities at the time of critical COVID-19 were linked to reduced mobility.
Researchers suggest surveillance for patients experiencing such symptoms is important regardless of pneumonia severity.
The study recommends continued assessment of patients after their hospital discharge.
Article: As long COVID turns three, Americans play disability roulette - The Boston Globe
SUMMARY:
Almost 1 in 10 Americans catching COVID this week, including previously healthy, vaccinated individuals, will be left lastingly ill. Long COVID-19 is an ongoing mass disability event, with 10 million Americans suffering from memory loss, heart problems, dizziness, and extreme fatigue, among others.
Patients with long COVID often fall through the cracks and are let down by physicians.
The long COVID, medical, and scientific communities are frustrated by the government's delay in providing relief and support.
Research
DEFINITIONS:
Obstructive sleep apnea (OSA): a sleep disorder characterized by the repetitive collapse of the upper airway during sleep, resulting in breathing cessation or marked reduction in airflow.
SUMMARY:
A preexisting obstructive sleep apnea (OSA) diagnosis may increase the risk of post-acute sequelae of SARS-CoV-2 infection (PASC).
This study used data from electronic health records to investigate the association between pre-coronavirus disease OSA diagnoses and PASC.
The study found that individuals with a pre-coronavirus disease OSA diagnosis were more likely to experience PASC.
The authors recommend that clinicians should consider OSA as a risk factor for PASC and monitor patients with OSA for longer-term COVID-19 outcomes.
DEFINITIONS:
The innate immune system recognizes initial infection and triggers a response, which can suppress infection effectively in most subjects.
SUMMARY:
This article is a summary of the many immunologic findings of the RECOVER initiative’s “Mechanistic Pathways Task Force”
PASC, or long COVID, is a growing concern due to prolonged symptoms after SARS-CoV-2 infection.
Studies show that immune responses play a role in the severity and outcomes of initial infection and subsequent PASC.
The specific mechanisms of immune dysregulation in PASC are yet to be defined, but understanding them is crucial for developing prevention and treatment strategies.
A bunch of interesting things highlighted here
Persistent or abnormal activation of proinflammatory pathways in tissue-specific macrophages could also have a role in the plethora of PASC symptoms involving multiple organ systems that is seen in these patients.
Multiple mechanisms likely underlie the production of autoantibodies in patients with severe COVID-19 manifestations.
My Take:
The focus on immune mechanisms in this article is important for understanding the dysregulation of immune processes in both acute COVID-19 and PASC.
The fact that there are certain mechanisms of immune dysregulation that are specific to PASC underscores the importance of further research
DEFINITIONS:
microglia: a type of cell in the brain responsible for synaptic structuring and maintenance
neurogenesis: the formation of new neurons in the adult brain
SUMMARY:
The hippocampus, which is important in memory… is recognized as one of the earliest and most distressed configurations of the brain throughout acute or chronic inflammatory circumstances owing to its specific susceptibility to neuroinflammatory incidents.
COVID-19, which activates microglia in the hippocampus and induces a CNS cytokine storm, leading to the loss of hippocampal neurogenesis.
The functional and structural changes in the hippocampus of COVID-19 patients can explain neuronal degeneration and reduced neurogenesis in the human hippocampus
Article: JCI - Prevalence and functional profile of SARS-CoV-2 T cells in asymptomatic Kenyan adults
DEFINITIONS:
Sero-: relating to serums or blood serum.
T cells: A type of lymphocyte responsible for cell-mediated immunity that differentiates into several cell types after exposure to antigens.
SUMMARY:
SARS-CoV-2 infection is less severe in Africa and has largely asymptomatic spread.
In this study, researchers show that 78% of individuals living in two rural regions of Kenya who had no reported respiratory symptoms since December 2019 and who were never knowingly in contact with individuals infected with SARS-CoV-2, possessed broadly reactive T cells specific to multiple SARSCoV-2 proteins.
Sixty percent of these asymptomatic individuals lacked anti-spike antibodies
The high incidence of T cell responses against different SARS-CoV-2 proteins in largely seronegative participants suggests that serosurveys underestimate SARS-CoV-2 prevalence.
Genetic or environmental factors play a role in the development of protective antiviral immunity.
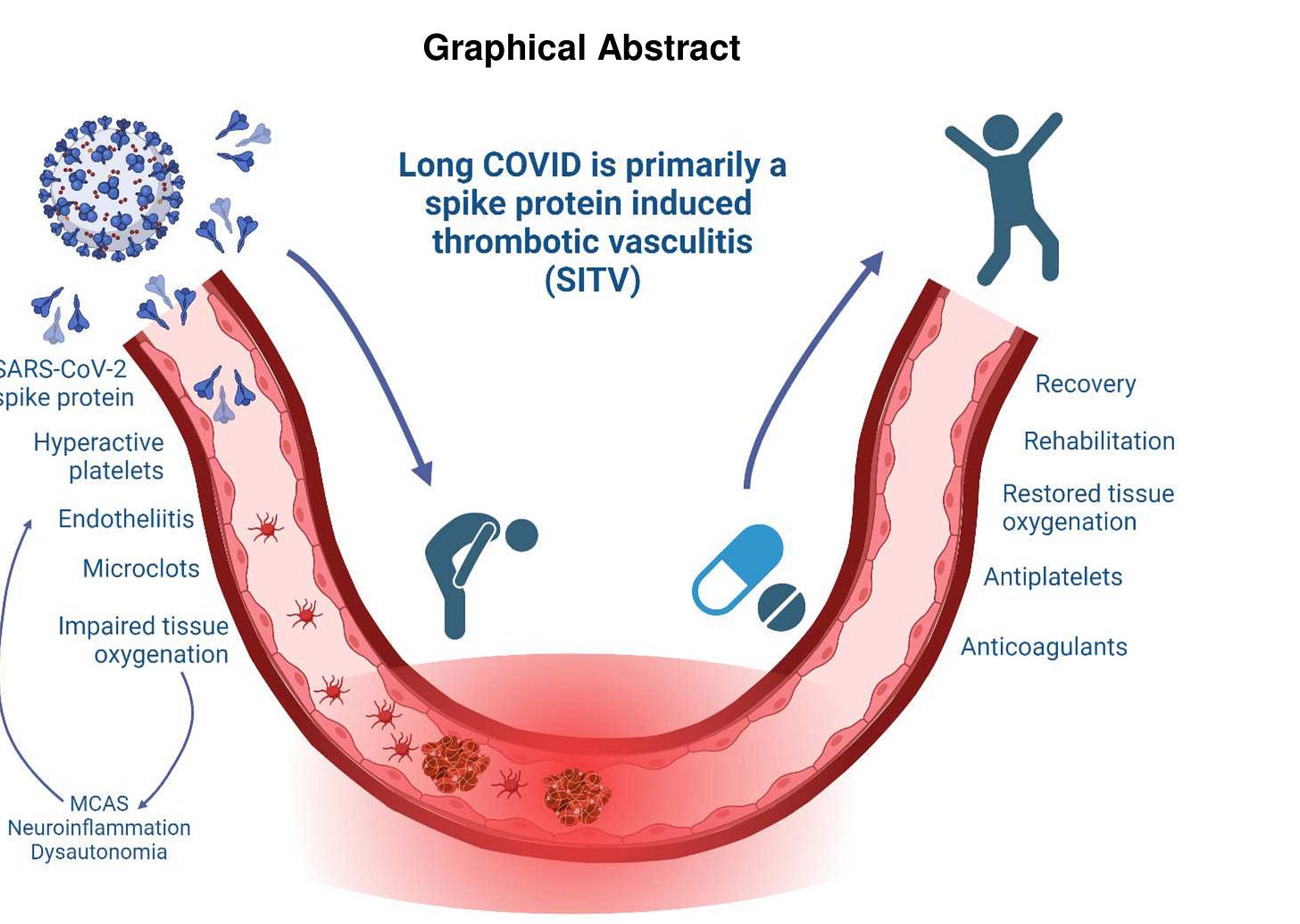
Article: Long COVID is primarily a Spike protein Induced Thrombotic Vasculitis | Research Square
DEFINITIONS:
Spike protein: a protein found on the surface of the SARS-CoV-2 virus that helps the virus to enter host cells.
Thrombotic Vasculitis: inflammation and clotting of blood vessels.
SUMMARY:
The authors hypothesize that:
Long COVID is a continuation of acute COVID-19 pathology driven by coagulopathy.
The SARS-CoV-2 spike protein can independently induce fibrinaloid microclots, platelet activation, and endotheliitis.
Persistent spike protein may be a key mechanism driving the continued coagulopathy in Long COVID.
Combination anticoagulant and antiplatelet drugs may bring significant relief to many Long COVID patients.
Authors believe that Long COVID should be referred to as Spike protein Induced Thrombotic Vasculitis (SITV).
My Take:
This preprint describes Long COVID as a continuation of acute COVID-19 pathology driven by coagulopathy, with the persistent spike protein being a key mechanism driving the continued coagulopathy.
DEFINITIONS:
Intrauterine hypoxia: a deficiency of oxygen reaching the fetus during pregnancy due to maternal conditions or other factors.
Perivillous fibrin deposition: a medical condition characterized by the accumulation of fibrin in the intervillous space of the placenta.
Epigenetic changes: modifications made to a gene that do not alter the underlying DNA sequence but affect gene expression.
SUMMARY:
The coronavirus disease 2019 (COVID-19) pandemic has led to an increase in maternal death rates and the requirement for intensive care treatment, including extracorporeal membrane oxygenation (ECMO), in severe acute respiratory syndrome coronavirus (SARS-CoV-2) infected mothers.
COVID-19 can also lead to stillbirth and is characterized by low blood oxygen in mothers, which may affect the placenta and fetus.
Fetal survivors of SARS-CoV-2 placentitis may have an increased risk of cardiovascular diseases in later life due to the effects of intrauterine hypoxia and maternal disease processes on the fetus.
SARS-CoV-2 placental infection likely has long-lasting effects on survivors.
My Take:
The article proposes that the virus may have an adverse effect on the cardiovascular health of surviving fetuses, similar to the effects of intrauterine hypoxia resulting from maternal cardiovascular diseases such as cyanotic heart disease, heart failure, or pulmonary hypertension
Thus, it is crucial to study long-term effects and prepare for future medical care when dealing with a pandemic.
Long COVID & Fatiguing Illness Recovery Program Monthly Session 2023-04-13
SUMMARY:
Project ECHO’s Long Covid & Fatiguing Illness Recovery Program hosts monthly educational sessions. Sessions are directed toward primary care providers, but all are welcome, including patients
April’s session was a research update on microclots, featuring researchers David Putrino, PhD, Resia Praetorius PhD, Douglas Kell PhD, Douglas Fraser PhD, Martin Krater PhD.
The scientists presented major findings from their research, including the pathobiology of Long Covid; platelets, circulating inflammatory molecules, and abnormal blood clotting; Long Covid plasma proteome; and deformability of blood cells.
If you enjoy this session, you may sign up for others here: https://hsc.unm.edu/echo/partner-portal/echos-initiatives/long-covid-fatiguing-illness-recovery/
Hope
Article: Breathing New Life: Oxygen Therapy Improves Heart Function in Long COVID Patients
DEFINITIONS:
Hyperbaric oxygen therapy (HBOT) involves inhalation of 100% pure oxygen at high pressure to increase delivery to the body’s tissues, which is particularly beneficial for tissues that are starved of oxygen due to injury or inflammation.
Global longitudinal strain (GLS) is a measure of the heart’s ability to contract and relax lengthwise and can help detect early signs of heart disease.
SUMMARY:
A small randomized trial has found that hyperbaric oxygen therapy (HBOT) may help restore proper heart function in patients with post-COVID syndrome, with HBOT participants experiencing a significant increase in global longitudinal strain (GLS), an indicator of heart function.
Hyperbaric oxygen therapy can be beneficial in patients with long COVID, according to Professor Marina Leitman of the Sackler School of Medicine.
The study enrolled 60 post-COVID syndrome patients with ongoing symptoms for at least three months after having mild to moderate symptomatic COVID-19 confirmed by a PCR test.
Echocardiography was used to assess left ventricular global longitudinal strain (GLS) which is a measure of a healthy heart's ability to contract and relax lengthwise.
My Take:
Though more research is needed to determine the optimal number of sessions for maximum therapeutic impact, the findings suggest that HBOT can help promote recovery of cardiac function in post-COVID syndrome patients.
I have heard mixed things about HBOT from different people who have tried it.





You might want to listen to the”POTScast” episode 127, available on Spotify- very interesting interview with Dr Federowski, worlds foremost leading researcher on POTS - plasma proteins in POTS patients are substantially different than control subjects, causes microclots. He’s also researching LC/POTS link. I’ve found the POTScast to be extremely informative, helpful- especially since LC, POTS, MCAS, me/CFS are all sort of intertwined and overlap. Highly recommend!
There appears to be so many studies going on, albeit perhaps small and underfunded. When government agencies recognise the problem and invest in it, we might have some real answers.
It’s very difficult being left without recognition, support or validation.
Do you think, from your vast readings of all the research papers, that they will find an answer or treatment that will be accepted and supported by doctors?