Long Covid Weekly #54: We need more Long Covid Trials, immune system findings in ME/CFS & more
Hi Everyone!
In this issue, we explore the current status of long Covid trials, shedding light on the need for further research and potential treatments. We also delve into the financial strains experienced by long Covid sufferers, uncovering the correlation between the condition and increased disability rates. Additionally, we delve into the molecular mechanisms responsible for the diabetogenic effects of Covid-19 infection and the utility of serum ferritin as a predictor for long Covid.
Media
Article: Where are the long COVID trials? - The Lancet Infectious Diseases
SUMMARY:
There is a desperate need for long COVID treatments.
Although estimates vary quite widely between populations and studies and depending on the definitions and methods used, 1 in 10 people experiences long COVID after infection.
The number and pace of clinical trials to tackle long COVID are vastly insufficient.
There is a long list of potential treatments, including antivirals, immunomodulators, anticoagulants or platelet inhibitors, and modulators of metabolism, neurological function or other organ-specific functions
My Take:
(Purely anecdotal) Although I agree things are moving far too slowly, it seems like trials are at least starting to pick up!
DEFINITIONS:
Safety-net programs: refer to government programs that provide assistance and support to individuals and families who are financially vulnerable or facing hardship.
Examples include programs like Medicaid, food assistance programs, and housing assistance.
SUMMARY:
The physical difficulties caused by long COVID are translating into severe financial hardships that include loss of work, utility shutoffs and trouble making rent or mortgage payments, new research shows.
One in 10 adults with long COVID say they stopped working because of their symptoms, according to an Urban Institute study based on a survey conducted late last year.
Over 40% of people with long COVID report having inadequate food for their household, the research shows, compared with 20% of adults who have had COVID-19 but do not have long COVID.
Difficulties paying the rent or mortgage and utility bills were also far more common among people with long COVID than those without, the researchers found.
Lack of access to paid sick leave is driving many patients with long COVID to cut back on other activities so that they can continue working, which can also add to financial strains if people need to pay for child care or other services, researchers say.
My Take:
Addressing these financial hardships is crucial for the recovery and well-being of those affected by long COVID.
Remote work being taken away by many companies is a terrible thing for those with Long Covid
SUMMARY:
During the COVID-19 pandemic era, more than 3 million people over the age of 18 have so far come forward with disabilities, and many more are expected to follow.
The COVID-19 pandemic has disproportionately afflicted disabled individuals and created a whole new group of disabled people.
Health care systems often failed disabled people during the pandemic, providing inferior care and struggling with accommodating their disabilities.
Disabled individuals also struggle with societal intolerance and face poverty at nearly twice the rate of their nondisabled counterparts.
Research
DEFINITIONS:
Natural killer (NK) cells: innate lymphoid cells that play a role in immunosurveillance and elimination of target cells.
Transient receptor potential (TRP) superfamily: a group of ion channels that detect environmental stimuli and mediate adaptive cellular responses, including regulation of intracellular calcium levels.
TRPM7: a member of the TRP superfamily that regulates calcium and magnesium homeostasis and is involved in various cellular processes.
Calcium (Ca2+): an important signaling molecule that plays a role in numerous cellular processes.
SUMMARY:
Impaired natural killer (NK) cell cytotoxicity is a consistent feature of ME/CFS.
TRPM7, a member of the transient receptor potential (TRP) superfamily of calcium (Ca2+) channels, plays a role in cellular processes such as immune function and regulation of intracellular Ca2+ levels.
This pilot study investigated the TRPM7-dependent Ca2+ influx in NK cells of ME/CFS patients and found altered TRPM7-mediated Ca2+ responses compared to healthy controls.
The findings suggest dysregulation of TRPM7 function in NK cells may contribute to the pathomechanism of ME/CFS.
My Take:
This study provides further evidence of immune dysfunction in ME/CFS through the investigation of TRPM7-mediated calcium responses in NK cells.
The altered TRPM7-dependent calcium influx observed in ME/CFS patients suggests a potential role for TRPM7 in the pathomechanism of the condition.
Further research is needed to better understand the underlying mechanisms and potential therapeutic targets related to TRPM7 and immune dysfunction in ME/CFS.
Be very curious if anyone in the community knows how this might be contributing to the development of ME/CFS
SUMMARY:
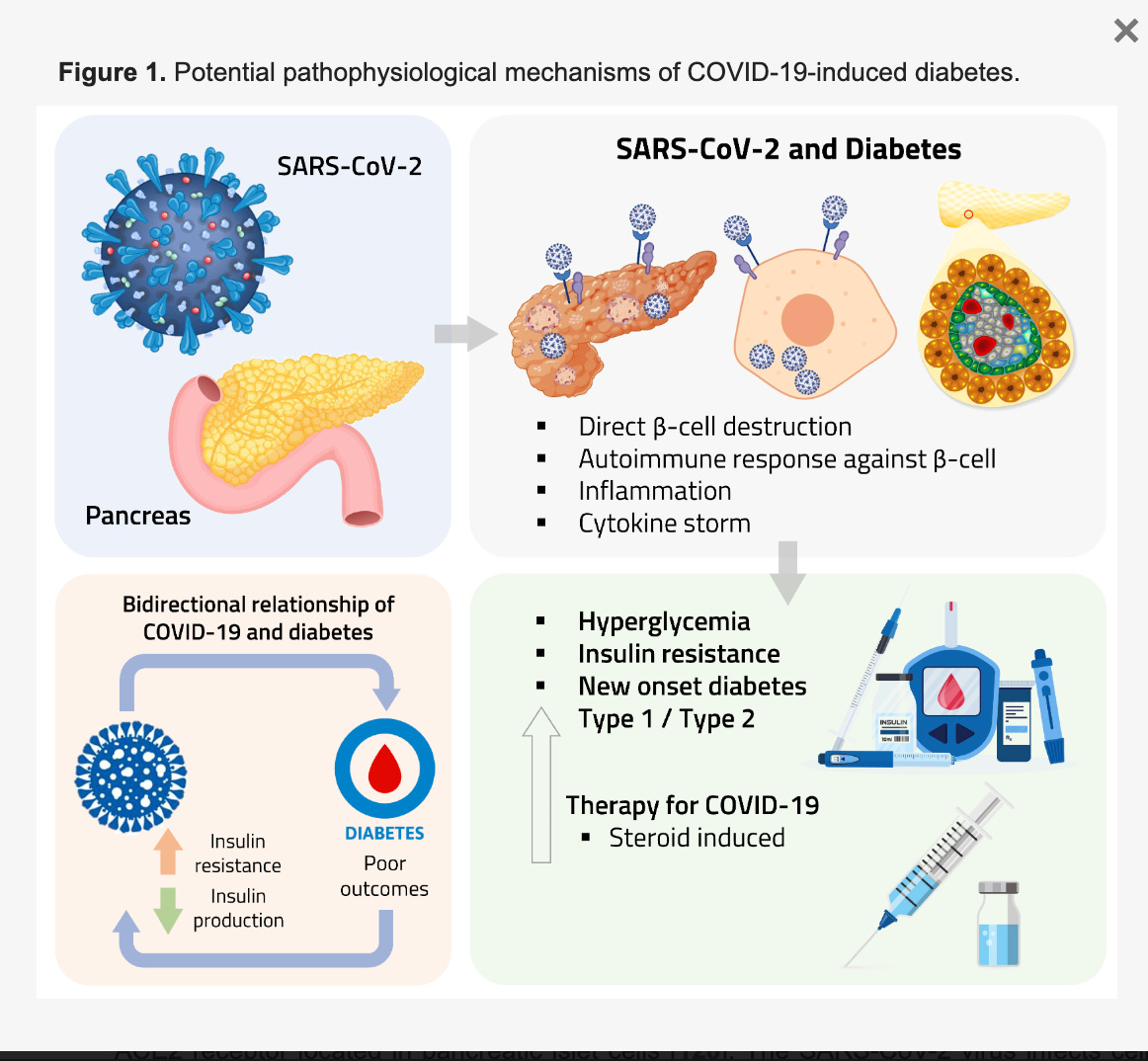
The COVID-19 pandemic has revealed a significant association between SARS-CoV-2 infection and diabetes, whereby individuals with diabetes are more susceptible to severe disease and higher mortality rates.
The pathogenesis of SARS-CoV-2-induced new-onset diabetes is complex and not yet fully understood.
it may involve direct 𝛽-cell damage, systemic-inflammation-induced insulin resistance, and hormonal dysregulation.
Additionally, treatment with glucocorticoids for COVID-19 may increase the risk of new-onset diabetes due to their association with hyperglycaemia and insulin resistance
Additionally, the connection between the 𝛽-cells and the endothelium, which is crucial for intact 𝛽-cell function, may also contribute to 𝛽-cell dysfunction indirectly.
Recent findings suggest a reciprocal relationship between COVID-19 and diabetes, wherein COVID-19 may contribute to developing new-onset diabetes and worsen existing metabolic abnormalities.
DEFINITIONS:
Ferritin: A protein that stores iron and releases it in a controlled manner as needed by the body.
SUMMARY:
Serum ferritin levels were about two times higher in patients with long COVID (particularly in women) who thereafter developed ME/CFS than in patients with long COVID who did not develop ME/CFS.
Ferritin synthesis is regulated by oxidation and anti-oxidation and is essential for in vivo inflammation and iron metabolism.
In the chronic phase of COVID-19, hyperferritinemia may be caused by iron dyshomeostasis.
Hyperferritinemia in long COVID may be related to accompanying hypertension, sleep disturbances, or depression.
My Take:
This suggests that hyperferritinemia may be a possible predictor of ME/CFS related to long COVID.
However, more research is needed to understand the underlying mechanisms and further validate these findings.
This is the first time I have ever heard of this relationship, super interesting.
DEFINITIONS:
Genome Wide Association Study (GWAS): a type of study that looks at many genetic variants across a population to see if any variant is associated with a particular trait or disease.
Mendelian Randomization (MR): a method that uses genetic variants as instrumental variables to assess the causal relationship between an exposure and an outcome.
SUMMARY:
This study obtained instrumental variables of 211 GM taxa from the Genome Wide Association Study (GWAS) to assess the effect of gut microbiota on ME/CFS risk.
Genus paraprevotella and genus Ruminococcaceae_UCG_014 were found to have a positive causal relationship with ME/CFS.
The findings of this study suggest that the composition of the gut microbiota is closely related to ME/CFS and provide new insights for further understanding the developmental mechanisms of the disease.
My Take:
This study provides evidence of a causal relationship between specific gut microbiota and ME/CFS.
There is quite a bit of research involving the two but has been all over the place from what I remember
The identification of these specific bacterial strains as risk factors for ME/CFS could potentially lead to the development of new diagnostic markers and therapeutic interventions for the disease.
As a data scientist interested in Causal Inference, I found this to be a thought-provoking piece of research!
DEFINITIONS:
Hepatocyte Growth Factor (HGF): a protein that plays a role in cell growth, tissue repair, and the coagulation process.
SUMMARY:
COVID-19 survivors may develop long-term health problems, including blood coagulation issues such as stroke and pulmonary embolism.
The immune response to SARS-CoV-2 infection produces pro-inflammatory cytokines that stimulate the production of hepatocyte growth factor (HGF), which plays a role in the coagulation process.
Currently, there is no information on the effect of SARS-CoV-2 infection on serum HGF concentrations in long COVID-19 survivors.
This review discusses the pathophysiology between COVID-19 and HGF, interleukin-6 (IL-6), and D-dimer as potential biomarkers for coagulation and inflammation.
HGF, also known as the scatter factor, plays a crucial role in various biological processes, including the blood clotting system.
While HGF is not directly involved in blood clotting itself, it influences several factors and pathways that regulate the process.
HGF promotes endothelial cell proliferation and migration, leading to the formation of new blood vessels.
This angiogenic effect is essential during wound healing and tissue repair, where the development of new blood vessels is crucial for delivering oxygen and nutrients.
My Take:
Identifying biomarkers such as HGF, IL-6, and D-dimer can help in diagnosing and monitoring coagulation and inflammation in COVID-19 patients.
DEFINITIONS:
Ehlers-Danlos syndrome (EDS): a group of connective tissue disorders characterized by joint hypermobility, skin laxity, and other symptoms.
SUMMARY:
A substantial fraction of individuals with joint hypermobility may have symptoms of Ehlers-Danlos syndrome (EDS), which is characterized by connective tissue dysplasia.
EDS patients often experience symptoms such as joint pain, skin laxity, chronic fatigue, and bowel irregularity, which can overlap with the symptoms observed in individuals with long COVID-19.
EDS and long COVID-19 share underlying mechanisms of articulo-autonomic dysplasia, which involve alterations in neuro-autonomic, immune, and inflammatory processes.
Comparison of EDS to COVID-19 included 15 overlapping dysautonomia–musculoskeletal symptoms in those with persisting symptoms and 24 identical or similar genes among the 84 moderating the severity of acute infection.
These many gene changes are hypothesized to act through a network or entome to produce overlapping Ehlers–Danlos or long COVID-19 syndrome profiles, their disease symptoms (canopy), genes (rhizome), and connecting pathogenetic mechanisms (trunk-phloem) visualized as entomes by analogy to Tolkien’s Ents.
My Take:
It seems like there has been a lot of research recently tying genetic factors, and the microbiome (individually). I would be interested in research looking at both concurrently.
DEFINITIONS:
IDO2: is one of the initial and rate-limiting enzymes of the kynurenine pathway of tryptophan catabolism, which is an essential amino acid and a precursor for several important compounds in the human body, such as serotonin and melatonin.
SUMMARY:
The abundant expression of the tryptophan-catabolizing enzyme indoleamine 2,3-dioxygenase-2 (IDO2) in fatal/severe COVID-19, led us to determine, in an exploratory observational study, whether IDO2 is expressed and active in PASC, and may correlate with pathophysiology
SARS-CoV-2 infection triggers long-lasting IDO2 expression
IDO2 expression is driven by the aryl hydrocarbon receptor (AHR) and coincides with an altered cellular metabolism, reflected by attenuated mitochondrial functioning and autophagy.
An explorative trial in PASC to interfere with the AHR-IDO2 pathway is warranted. As there are no potent inhibitors of IDO2 available for use in humans, an AHR antagonist is a likely therapeutic option.
Hope
Article: Study finds that a 100-year-old treatment inhibits COVID-19 infection
DEFINITIONS:
ACE2: the receptor that the SARS-CoV-2 virus uses to enter human cells.
Heparan sulfate: a molecule present on the cell surface that also facilitates the entry of the virus into cells.
SUMMARY:
A team of researchers led by Rensselaer Polytechnic Institute's Jonathan S. Dordick, Ph.D., has found that the 100-year-old drug suramin inhibits the infection of SARS-CoV-2, the virus that causes COVID-19.
Suramin binds to the ACE2 and cell surface heparan sulfate binding sites on the spike protein of the virus, preventing it from infecting cells.
My Take:
Suramin's ability to target the binding sites on the virus's spike protein, as well as its broader mechanism of action, make it a promising candidate for antiviral therapy.
Further research and studies are needed to fully evaluate the effectiveness of suramin as a COVID-19 therapeutic or prophylactic measure.



I have hEDS, and noticed early on that people with long Covid were basically experiencing EDS symptoms, which terrified me. I figured it would make people who already had EDS (1 in 200 people by more recent estimates) sicker.
That has played out in my own experience with MCAS getting much worse. MCAS destabilizes connective tissue. And I would say that over 95% of people with hEDS that I’ve talked to have also had a worsening of symptoms post Covid.
DR CHANG DOES INFO ON ME/CFS
Gut tissues can retain SARS-CoV-2 particles after COVID-19 infection for more than one year after the resolution of COVID-19
👇
WRONG TEST MAN
Gustavo Aguirre Chang
https://twitter.com/Aguirre1Gustavo/status/1608786500988305411
UNDIAGNOSED VIRAL PERSISTENCE
IN 32.5% OF PATIENTS UNDERGOING BARIATRIC SURGERY
All had Negative PCR before Surgery
They were unaware they had a Persistent Infection due to SARS-CoV-2
One part had more than 1 year since infection
Are undiagnosed Long Covid
Lingering SARS-CoV-2 in Gastric and Gallbladder Tissues of Patients with Previous COVID-19 Infection Undergoing Bariatric Surgery
https://link.springer.com/article/10.1007/s11695-022-06338-9